Imaging group
News of the group:
(October 1, 2021)
Brain Imaging in Psychiatry Program:
In collaboration with the Neurospin neuroimaging platform (CEA Saclay), we contribute to the description of the neuroanatomical and neurofunctional bases associated with the most disabling psychiatric pathologies. We are particularly interested in the brain substrates associated with emotional dysregulation and negative symptoms in psychiatric disorders such as bipolar disorder, schizophrenia and autism spectrum disorders (Sarrazin et al., 2014; Favre et al., 2019; Laidi et al, 2019; d’Albis et al, 2018). For this, we use both innovative imaging techniques (e.g., 7 Tesla MRI) as well as very large subject samples (sometimes several thousand).
Our work has shown abnormalities in white and gray matter structure in patients with bipolar disorder (Houenou et al., 2007; Sarazin et al., 2014; Favre et al., 2019; Laidi et al., 2021) that appear to be ameliorated in patients taking lithium (Favre et al., 2019; Hozer et al., 2021; Sarrazin et al, 2019, 2021) and after psychoeducation (Favre et al., 2016). In autism spectrum disorders, we have been able to identify brain correlates of social cognition disorders (d’Albis et al., 2018; Hotier et al., 2017).
With a better understanding of the brain substrates underlying the symptoms, we aim to use MRI to predict the response to commonly prescribed treatments (lithium, antipsychotics, antidepressants). We are developing and evaluating the therapeutic value of innovative brain stimulation techniques such as rTMS (transcranial magnetic stimulation), tDCS (direct current stimulation) and neurofeedback to improve the management of these disorders. We are initiating a randomized, double-blind clinical trial using functional MRI neurofeedback to treat residual symptoms of bipolar mood disorder.
Brain morphology abnormalities in bipolar disorder
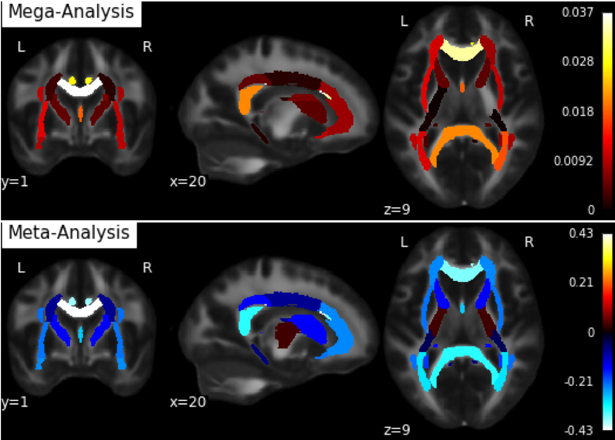 A) White matter microstructure: results of a comparison of diffusion MRI data from 3033 subjects including 1482 patients with bipolar disorder and 1551 healthy controls and from 26 different studies (12 countries) performed in collaboration with the ENIGMA consortium (Favre et al., 2019). We found diffuse abnormalities in anatomical connectivity, particularly affecting the corpus callosum and cingulate.
A) White matter microstructure: results of a comparison of diffusion MRI data from 3033 subjects including 1482 patients with bipolar disorder and 1551 healthy controls and from 26 different studies (12 countries) performed in collaboration with the ENIGMA consortium (Favre et al., 2019). We found diffuse abnormalities in anatomical connectivity, particularly affecting the corpus callosum and cingulate.
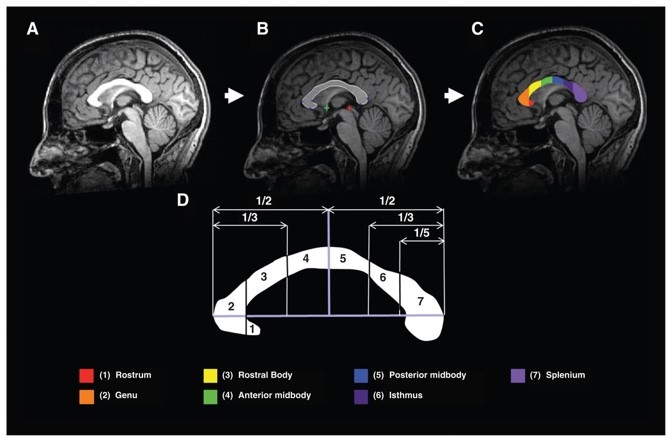 B) Corpus callosum volumes: results from comparison of structural MRI data (T1) of 318 subjects including 172 patients with bipolar disorder type I and 146 controls and from 4 different centers (4 countries) (Sarrazin et al., 2015). We found that bipolar patients had smaller areas of corpus callosum than controls along the posterior, isthmus, and splenium. In addition, patients with a history of psychotic symptoms showed a larger area of the rostral region of the corpus callosum compared to those without a history of psychotic features. Given the large sample size of these studies, these brain abnormalities may represent a robust biomarker for bipolar disorder. They shed light on the pathophysiology of this disorder by showing that structural abnormalities affect the entire brain and particularly the corpus callosum in patients with a history of psychotic symptoms.
B) Corpus callosum volumes: results from comparison of structural MRI data (T1) of 318 subjects including 172 patients with bipolar disorder type I and 146 controls and from 4 different centers (4 countries) (Sarrazin et al., 2015). We found that bipolar patients had smaller areas of corpus callosum than controls along the posterior, isthmus, and splenium. In addition, patients with a history of psychotic symptoms showed a larger area of the rostral region of the corpus callosum compared to those without a history of psychotic features. Given the large sample size of these studies, these brain abnormalities may represent a robust biomarker for bipolar disorder. They shed light on the pathophysiology of this disorder by showing that structural abnormalities affect the entire brain and particularly the corpus callosum in patients with a history of psychotic symptoms.
Selected publications
d’Albis, M. A., Guevara, P., Guevara, M., Laidi, C., Boisgontier, J., Sarrazin, S., ... & Houenou, J. (2018). Local structural connectivity is associated with social cognition in autism spectrum disorder.
Brain, 141(12), 3472-3481.Favre, P., Pauling, M., Stout, J., Hozer, F., Sarrazin, S., Abe, C., ... & Houenou, J. (2019). Widespread white matter microstructural abnormalities in bipolar disorder: evidence from mega-and meta-analyses across 3033 individuals.
Neuropsychopharmacology, 44(13), 2285-2293.Favre, P., Houenou, J., Baciu, M., Pichat, C., Poupon, C., Bougerol, T., & Polosan, M. (2016). White matter plasticity induced by Psychoeducation in bipolar patients: a controlled diffusion tensor imaging study.
Psychotherapy and psychosomatics, 85(1), 58-60.Hotier, S., Leroy, F., Boisgontier, J., Laidi, C., Mangin, J. F., Delorme, R., ... & Houenou, J. (2017). Social cognition in autism is associated with the neurodevelopment of the posterior superior temporal sulcus.
Acta Psychiatrica Scandinavica, 136(5), 517-525.Houenou, J, Wessa, M., Douaud, G., Leboyer, M., Chanraud, S, Perrin, M, Poupon, C, Martinot, J.-L, Paillere-Martinot, M.-L. (2007) Increased white matter connectivity in euthymic bipolar patients: Diffusion tensor tractography between the subgenual cingulate and the amygdalo-hippocampal complex
Molecular Psychiatry, 12 (11): 1001-10Hozer, F., Sarrazin, S., Laidi, C., Favre, P., Pauling, M., Cannon, D., ... & Houenou, J. (2021). Lithium prevents grey matter atrophy in patients with bipolar disorder: an international multicenter study.
Psychological medicine, 51(7), 1201-1210.Laidi C, D’albis Ma, Wessa M, Linke J, Phillips M, Delavest M, Bellivier F, Versace A, Almeida J, Sarrazin S, Poupon C, Le Dudal K, Daban C, Hamdani N, Leboyer M, Houenou J (2015 Cerebellar Volume in Schizophrenia and Bipolar I Disorder with and without Psychotic Features.
. Acta Psychiatrica Scandinavica, 131(3), 223-233.Sarrazin S, Poupon C, Uszynski I, Teillac A, Mangin Jf, Polosan M, Favre P, Laidi C, D'albis Ma,Leboyer M, Lledo Pm, Henry C, Emsell L, Shakeel Mk, Goghari Vm, Houenou J. (2020) Neuroimaging Evidence for Increased Neurite Density in Patients Taking Lithium: A Replication Study.
Psychother Psychosom, 90(1):71-72.Sarrazin S, Poupon C, Linke J, Wessa M, Phillips M, Delavest M, Versace A, Almeida J, Guevara P, Duclap D, Duchesnay E, Mangin JF, Le Dudal K, Daban C, Hamdani N, D’Albis MA, Leboyer M, Houenou J.(2014) A multicenter tractography study of deep white matter tracts in bipolar i disorder : psychotic features and interhemispheric disconnectivity.
JAMA Psychiatry, 71(4):388-96